 Healthcare leaders today are operating in one of the most complex environments the industry has ever faced. Margins are thin, workforce shortages persist, cybersecurity threats are constant, and regulatory pressures continue to grow. At the same time, patients and families who now live in a digital world expect healthcare to function with the same convenience, transparency, and responsiveness offered by digitally enabled technologies which they experience in other industries.
Healthcare leaders today are operating in one of the most complex environments the industry has ever faced. Margins are thin, workforce shortages persist, cybersecurity threats are constant, and regulatory pressures continue to grow. At the same time, patients and families who now live in a digital world expect healthcare to function with the same convenience, transparency, and responsiveness offered by digitally enabled technologies which they experience in other industries.
I’d suggest that every healthcare strategy is now a digital strategy. That doesn’t mean that healthcare will become a technology industry. Healthcare will always be about patients, families, clinicians, and caregivers. Digital capabilities, however, now are essential elements for how healthcare organizations operate, compete, and deliver care. Whether addressing access, value-based reimbursement, workforce efficiency, patient and family engagement, or operational performance, technology is increasingly the enabler of success.
Digital is not the same old IT we used to explain using simple metaphors describing it as the skeleton or nervous system of an organization. Today, digital IT is more like the mRNA of a healthcare organization impacting all aspects of the operating model that is a part of every activity in the organization.
Strategy Has Changed and So Has the Speed of Change
For decades, healthcare organizations approached strategy with fairly predictable planning cycles. There were one-year operational and financial plans, three-year strategic plans, and five-year or longer roadmaps. Those timelines are too long and too limited in our digital world. Today the pace of technological and market change has compressed strategic planning horizons dramatically. The new practical planning horizons should be:
- Immediate priorities,
- One-year initiatives, and
- Two-to-three-year transformations
Why? Because digital innovation moves faster than traditional healthcare planning processes. New technologies emerge quickly. Consumer expectations shift rapidly. New competitors continue to target and enter the healthcare space. Healthcare organizations can no longer treat digital transformation as a long-term project. It has become a continuous and evolving strategic capability. Agility, flexibility, and the capacity for continuous self-reinvention have become core competencies for every healthcare organization.
Data are Still Healthcare’s Most Underutilized Assets
Healthcare organizations now collect and generate vast volumes of data including clinical, operational, financial, and consumer data. Yet many organizations still struggle to transform that data into meaningful insights. Here’s a chart I developed for a course I teach describing my proposed version of a Data Transformation Model where transformation occurs at every step as you move from start (data) to finish (widespread utility) on the model:
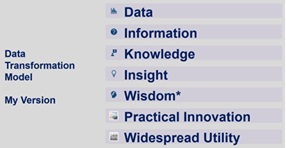
*Practical wisdom is “knowing what is good, right, or best, given a particular set of circumstances” – Aristotle (paraphrased)
The ideal goal is to create widespread utility. Most healthcare organizations have mastered the first step. They collect enormous amounts of data. The challenge and opportunity is moving down the model. Organizations that succeed in the coming decade will be those that transform raw data into actionable insights that improve clinical decision-making, operational performance, and patient outcomes.
A Philips report suggested, “Healthcare organizations often possess vast amounts of data but lack the insights needed to improve care and efficiency”[1]. Simply put, data without insight creates digital clutter. Practical wisdom should inspire practical innovations that can be shared and utilized universally.
Artificial Intelligence Is Accelerating the Shift to Digital
Artificial intelligence is accelerating the integration of digital capabilities into healthcare strategies. AI is already improving healthcare in areas such as medical imaging, clinical documentation, predictive analytics, and revenue cycle management. The most important point, however, is that AI is not replacing clinicians but augmenting them. The most successful AI deployments treat technology as a thought partner that enhances human decision-making rather than attempting to replace it. Organizations that approach AI strategically through governance, clearly defined use cases, and measurable outcomes are already seeing improvements in efficiency, quality, and clinician satisfaction.
The CIO Role Is Evolving
As digital capabilities become central to enterprise strategy, the role of the CIO is evolving as well.
The days when CIOs were viewed primarily as infrastructure managers or application overseers are rapidly disappearing. Today’s CIO must operate as an enterprise strategist and transformational leader. Research by Gartner shows that organizations where CIOs partner closely with other executives to co-lead digital initiatives are significantly more likely to realize value from technology investments[2]. Digital transformation works best when it is shared leadership, not simply an IT initiative.
Innovation Requires Governance
Healthcare is experiencing a surge of digital innovation including AI demonstration projects (not pilots[3]), digital front doors, remote monitoring platforms, and new care delivery models. People are excited about the potential, but the demand can be overwhelming. Responsible management requires easily and widely understood “lightweight” governance. Innovation without governance often leads to fragmentation, duplication, and wasted investment. Successful organizations manage innovation with disciplined governance to ensure digital initiatives align with enterprise priorities. They measure outcomes carefully. Using a lightweight approach innovation should move quickly and strategically.
A Leadership Imperative
Healthcare leaders sometimes ask whether digital transformation is necessary or whether their organizations can afford to move cautiously. The reality is that digital transformation is already underway across healthcare and around the world. The real question is not whether it will occur, but whether organizations will lead it or be forced to react to it. Healthcare organizations that strategically develop digital capabilities will be far better positioned to navigate the challenges ahead.
In today’s healthcare environment, strategy and digital capabilities can no longer be separate discussions. They are inextricably connected. The organizations that recognize and act accordingly will shape the future of healthcare rather than struggle to keep up with it.
[1] Philips. Future Health Index 2024: Better Care for More People
[2] Gartner. CIO Agenda 2025: Top Priorities for CIOs
[3] The term “pilot” implies there is potential for failure. Using the term “demonstration” communicates confidence that the technology solution will be successful. Avoid the use of “fail fast”. Use “succeed swiftly” instead.
